The 4 stages of anaphylaxis actually move fast in minutes, sometimes within minutes of exposure to a trigger. Understanding these 4 stages of anaphylaxis isn’t just useful medical trivia. So, It’s the difference between catching a reaction immediately and ending up in a situation where just seconds matter. If someone in your household is reacting right now and you are confused about how serious it is, this guide will help you figure that out, quickly.
Anaphylaxis is not only a “really bad” allergic reaction. It’s a full-body immune system emergency, and knowing what to look for at each stage is the fastest way to know when you can wait, when you need to call 911, and when to just get in the car and head straight to the ER of Fort Worth.
What Is Anaphylaxis? (And Why It’s Not Just a Bad Allergic Reaction)
So what is anaphylaxis exactly? In simple terms, it’s a severe and potentially life-threatening allergic reaction, which actually happens when your immune system suddenly releases a surge of chemicals which cause your blood pressure to drop, your airways to swell, and widespread disruption across different body systems.
A normal allergic reaction stays local. You eat something with peanuts and you get a rash on your arm. What is anaphylaxis by contrast? It’s when that reaction goes systemic, hitting your skin, your lungs, your heart, and your gut simultaneously. That’s the distinction that makes it an emergency.
What is anaphylaxis doing inside your body?
When you come into contact with a trigger your immune system considers harmful, whether it’s a food, a medication, an insect sting, or in some cases even exercise, it sets off a powerful release of histamine and other inflammatory chemicals. As a result, blood vessels dilate and leak, airways swell and narrow, and blood pressure can fall quickly to dangerous levels.
Your body is not trying to hurt you. It’s overreacting in a way it was never designed to handle. And that overreaction is what makes every minute count once the more serious stages begin.
The 4 Stages of Anaphylaxis, What Each One Looks and Feels Like

Most medical descriptions of the 4 stages of anaphylaxis tell you what symptoms appear. What they often don’t tell you is what those symptoms actually feel like, which is the information that helps a scared person at home decide what to do. Here’s both.
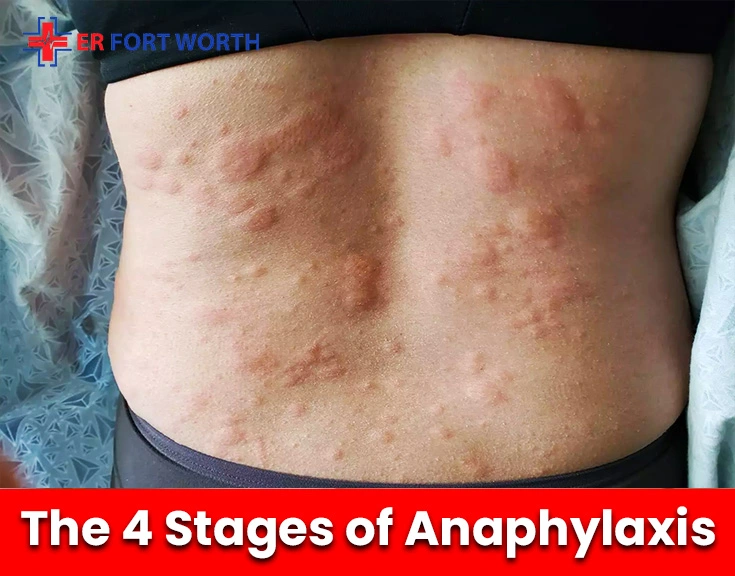
Stage 1 — Mild: Skin Changes and Itching
Stage 1 is easy to dismiss, that’s what makes it dangerous.
What you see: Hives (raised, red, blotchy welts), skin flushing, or localized itching, often starting at the point of contact. Maybe the lips look slightly puffy. Maybe there’s a patch of redness spreading across the neck or chest.
What it feels like: A tingling in the mouth after eating. An itch which spreads faster than a typical bug bite. Feeling warmth in the face that came out of nowhere. Patients often tell us, “I thought I was just hot.”
At this stage, someone with a known allergy and an EpiPen may be able to self-treat and monitor. But if there’s any doubt, or if progression happens, don’t wait.
Stage 2 — Moderate: Spreading Hives, Swelling, GI Distress
Stage 2 is where the reaction has stopped being a skin problem and has started being a body problem.
What you see: Hives are spreading. Lips and tongue are visibly swollen. The person may be rubbing their throat or complaining it feels “tight” or “scratchy.” Stomach cramping, nausea, or vomiting may begin.
What it feels like: “My throat feels like it’s closing.” “I feel sick to my stomach out of nowhere.” “My face feels huge.” The anxiety ramps up here too, not because the person is overreacting, but because their body is signaling danger.
This is the stage where most people should be in the car heading to an ER. If there’s an EpiPen available, use it and then come in anyway, epinephrine buys time, it does not end the reaction.
Stage 3 — Severe (Anaphylactic Shock): Breathing and Blood Pressure
It is the stage where anaphylaxis becomes immediately dangerous and life-threatening. The airway is also compromised at this. And blood pressure is rapidly falling. Your body is in anaphylactic shock at this stage.
What you see: Labored breathing, audible wheezing or stridor (a high-pitched sound when inhaling). Pale or bluish skin. Rapid, weak pulse. The person who is going through this may become confused, dizzy, or unable to stand.
What it feels like: “I can’t breathe.” “Everything went fuzzy.” “My heart is pounding but I feel like I’m going to pass out.” Patients with this stage often describe a feeling of impending doom, and that’s not a metaphor, it is a real and recognized symptom of anaphylactic shock.
Call 911 immediately. If there is an EpiPen and you have not used it so far, use it now. Do not drive the person to the ER if they’re in this condition, have emergency services come to you.
Stage 4 — Life-Threatening: Unconsciousness and Organ Failure
Stage 4 is a serious medical emergency without any ifs and buts. The person is losing or has lost consciousness. At this stage their airway may be completely blocked. And their blood pressure has dropped to a level where vital organs aren’t being perfused.
Stage 4 anaphylaxis can be fatal if there is no immediate treatment, IV epinephrine, airway management, fluid resuscitation, and intensive monitoring. This is exactly the scenario our team at the ER is equipped and available to handle the case 24/7.
The key takeaway across all four stages: anaphylaxis can progress from Stage 1 to Stage 4 in under 15 minutes. That’s why the earlier you act, the more options you have.
The 4 Stages of Anaphylaxis
| Stage | Severity | What You See | What It Feels Like | What To Do |
| Stage 1 | Mild | Hives, skin flushing, localized itching, slightly puffy lips | Tingling in the mouth, warmth in the face, an itch spreading faster than a bug bite | Use EpiPen if prescribed, monitor closely, don’t ignore it |
| Stage 2 | Moderate | Spreading hives, swollen lips and tongue, vomiting, throat feels scratchy | “My throat feels tight.” Sudden nausea, face feels swollen, rising anxiety | Use EpiPen and head to the ER now, don’t wait it out |
| Stage 3 | Severe (Anaphylactic Shock) | Wheezing, pale or bluish skin, weak rapid pulse, confusion, can’t stand | “I can’t breathe.” “Everything went fuzzy.” Feeling of impending doom | Call 911 immediately, do not drive yourself |
| Stage 4 | Life-Threatening | Loss of consciousness,airway blocked, organs not getting blood flow | Unresponsive, the person cannot communicate what they feel | 911 and ER only, every second counts |
Go to the ER Immediately, Red-Flag Symptoms You Cannot Ignore

If you experience any of the following in your body or in your loved one, just stop reading and head to the ER now immediately, or call 911. At this highly critical stage this is no longer wait-and-see territory:
- Difficulty breathing, wheezing, or a sense that the throat is closing
- Swelling of the lips, tongue, or throat
- Sudden drop in blood pressure (pale skin, dizziness, feeling faint)
- Chest tightness or pain
- Rapid or weak pulse
- Confusion, slurred speech, or extreme agitation
- Bluish or grayish color around the lips or fingernails
- Loss of consciousness or unresponsiveness
- Symptoms appearing in two or more body systems at once (e.g., hives + vomiting + throat tightness)
- Symptoms rapidly worsening after epinephrine administration
What CAN be monitored at home (temporarily, for a mild reaction only):
- Localized hives or itching that are stable, not spreading
- Mild skin flushing without any throat, breathing, or GI symptoms
- Reactions that were previously evaluated by a physician, with a known management plan in place
Even in a mild case: if you’ve used an EpiPen, come in. Biphasic anaphylaxis, a second wave of symptoms hours after the first, occurs in roughly 1 in 5 cases, and you need to be observed.
What About Idiopathic Anaphylaxis? When There’s No Obvious Trigger
One of the most frightening versions of this condition is idiopathic anaphylaxis, a full anaphylactic reaction with no identifiable cause. No food. No sting. No new medication. Nothing changed.
Idiopathic anaphylaxis accounts for a significant portion of anaphylaxis cases treated in ERs across the country, and it’s more common than most people realize. In idiopathic anaphylaxis, the immune system fires off a massive reaction without an obvious external trigger, and because there is no trigger to avoid, patients often feel like they’re living with a ticking clock.
If you’ve experienced idiopathic anaphylaxis, here’s what you need to know:
- It can recur. You should carry epinephrine at all times.
- You need a formal allergy workup, not to diagnose the trigger (there may not be one), but to rule out conditions like mastocytosis that can mimic idiopathic anaphylaxis.
- There are ongoing management protocols that allergists use to reduce recurrence risk.
- The ER is the right first stop for any acute episode. Long-term management should involve an allergist.
In North Texas and Tarrant County, we see idiopathic anaphylaxis year-round, and our team will treat the reaction, stabilize the patient, and make sure follow-up is in place before discharge.
Can I Die in My Sleep from Anaphylaxis?

This is one of the most common questions people search after having an anaphylactic reaction, and it deserves a direct, honest answer.
Can I die in my sleep from anaphylaxis? Yes, in rare but documented cases, fatal anaphylaxis has occurred during sleep, particularly in people with severe food allergies who had an accidental exposure before bed. The concern about whether you can die in your sleep from anaphylaxis is especially relevant for parents of children with known severe allergies, and for adults who have had prior reactions.
That said, a few things reduce this risk significantly:
- Using your EpiPen at the first signs of a reaction, do not wait to see if it passes
- Going to the ER after any epinephrine use, biphasic reactions can occur 4–12 hours later
- Having a clear action plan from your allergist
- If you had a reaction during the day and symptoms have resolved, consider being evaluated before sleep
If you’re asking “can I die in my sleep from anaphylaxis” because you had a reaction today and feel “mostly fine”, come in. That’s exactly the scenario we want to evaluate before you go to bed.
What Happens at the ER When You Come In for Anaphylaxis
A lot of people delay coming to the ER because they don’t know what to expect, or they’re worried about being seen as “overdramatic.” You are not being dramatic. Anaphylaxis is one of the few conditions where the window between manageable and critical closes fast.
Here’s what happens when you walk through our doors:
- Immediate triage, we assess airway, breathing, and circulation right away. Anaphylaxis gets flagged as high priority.
- Epinephrine, if not already given, is the first-line treatment. It reverses airway swelling and stabilizes blood pressure within minutes.
- IV access and fluids, to support blood pressure and allow rapid medication delivery. IV fluids are often critical in anaphylactic shock.
- Antihistamines and steroids, these are not the primary treatment, but they help reduce ongoing inflammation and lower the risk of a biphasic reaction.
- Monitoring period, typically 4–6 hours minimum after epinephrine to watch for biphasic reaction. Longer if the reaction was severe.
- Discharge planning, you’ll leave with a prescription for an epinephrine auto-injector (EpiPen) if you don’t have one, a referral for allergy follow-up, and a written action plan.
We don’t judge anyone for coming in when they weren’t sure. That’s what we’re here for.
A Note From Our Team in Fort Worth
In Tarrant County, we see anaphylaxis cases cluster around predictable patterns. Spring allergy season in North Texas is intense, the cedar, oak, and grass pollen counts here are among the highest in the country, and while pollen alone rarely causes anaphylaxis, patients with multiple sensitivities are at higher baseline risk. Summer brings insect sting reactions as families spend time outdoors. Fall and winter holiday gatherings mean more exposure to food allergens, hidden tree nuts in stuffing, shellfish in holiday spreads.
We also regularly see patients who delayed coming in because they felt better after using their EpiPen. That’s actually one of the more dangerous situations, epinephrine is fast but short-acting, and the reaction can roar back. If you’ve used your auto-injector anywhere in Fort Worth today, don’t wait. Head to us.
Our ER is open 24 hours a day, 7 days a week. No appointment. No waiting to see if it passes. If your gut says something is wrong, it probably is.
If you’re in Fort Worth and something doesn’t feel right, don’t wait for it to get worse. Anaphylaxis moves fast, and so do we. ER of Fort Worth is open 24 hours a day, 7 days a week, with no appointment needed. If you used an EpiPen today, if your throat feels tight, if your heart is racing and your skin is breaking out, come in now. We’d rather see you and send you home than have you wait and regret it.
Our Er Open 24/7, No Appointment Needed.