If you are trying to figure out how to treat seasonal allergies right now, chances are you or someone you love feels miserable, and you want real answers fast. Seasonal allergy symptoms can look a lot like other illnesses, and knowing which path to take, home treatment, urgent care, or the ER, can feel genuinely confusing. As someone who works in a Fort Worth emergency room, I want to walk you through what’s actually going on in your body, what you can manage at home, and when it’s time to come in.
Why Seasonal Allergies Happen?
When you breathe in something your immune system has decided it doesn’t like, pollen from cedar, oak, or ragweed, it releases a chemical called histamine. That histamine is the troublemaker. It triggers swelling, mucus production, itching, and inflammation throughout your upper respiratory tract. Your body thinks it’s fighting off an invader. It isn’t. But try telling that to your sinuses at 6am during allergy season in North Texas.
In Fort Worth and across Tarrant County, we deal with one of the more aggressive allergy calendars in the country. Mountain cedar hits hard in winter, oak and elm in early spring, grasses through late spring and early summer, and ragweed from late summer into fall. There’s barely a break. If it feels like allergy season is year-round here, that’s because it nearly is.
Seasonal Allergy Symptoms: What They Actually Feel Like

Most articles list seasonal allergies symptoms as a medical checklist. But when you’re in the thick of it, these symptoms have a very specific feel, one that patients describe to me regularly when they come in wondering if they have COVID, a sinus infection, or something worse.
Common seasonal allergy symptoms include:
- Sneezing, often in rapid bursts, especially in the morning or after stepping outside
- Runny or stuffy nose, clear, watery discharge is a classic allergy sign (thick, colored mucus points more toward infection)
- Itchy, watery, or red eyes, feels like grit that won’t wash out
- Itchy throat, roof of mouth, or ears, that maddening sensation that nothing scratches
- Postnasal drip, leads to a mild sore throat and persistent cough
- Fatigue, histamine and disrupted sleep take a toll
- Mild headache or facial pressure, from sinus congestion building up
Here’s the key distinction we use: seasonal allergy symptoms typically don’t include fever. If you’re running a temperature, that changes the picture entirely. You’re either fighting an infection, or your allergies have opened the door to one.
How to Treat Seasonal Allergies on your own

For most of our neighbors, the first line of defense happens at the local pharmacy or in the comfort of home.
1. Environmental Control
- The “Fort Worth Wash”: After spending time at Trinity Park or outdoors, shower and change clothes immediately. Pollen sticks to hair and fabric.
- Keep Windows Closed: It’s tempting on a rare 70-degree day, but your AC filter is your best friend during allergy season.
2. Over-the-Counter Options
- Antihistamines: These block the histamine response.
- Nasal Steroids: These reduce inflammation in the nasal passages but often take a few days of consistent use to work.
- Saline Rinses: Physically washing the allergens out of your sinuses can provide massive relief.
The Turning Point: Is It Just Allergies or Something Else?
One of the most common questions I get in the triage bay is: “How do I know this isn’t the flu or COVID?” While seasonal allergy symptoms can feel miserable, they usually follow a specific pattern that differs from an infection
When to Go to the ER Immediately ( Don’t Wait )

This is the section I want every parent, caregiver, and patient to read carefully. Most seasonal allergy symptoms are uncomfortable but manageable. Some are not. These are the signs that mean stop treating this at home and come in now:
- Difficulty breathing, wheezing, or tightness in the chest
- Throat swelling or a sensation that your airway is closing
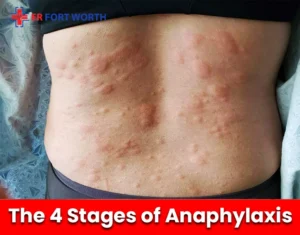
- Rapid, worsening hives, especially spreading to face, lips, or tongue
- Dizziness, confusion, or sudden weakness
- Bluish lips or fingertips (cyanosis)
- Loss of consciousness or near-fainting
- Anaphylaxis symptoms following exposure to a known allergen (bee sting, food, medication)
- Fever above 103°F or a fever in an infant under 3 months
- Symptoms in a young child or infant that are rapidly worsening
These aren’t classic allergy symptoms anymore, they are signs of a severe allergic reaction or a secondary complication. Our ER in Fort Worth is equipped to handle all of these. When in doubt, come in. It’s always better to be checked and sent home than to wait too long.
What You Can Safely Monitor at Home
Not every symptom needs an ER visit, and I’d rather give you a clear picture of both sides. If your symptoms fit this profile, it’s reasonable to continue home treatment and monitor:
- Clear runny nose, sneezing, and itchy eyes with no fever
- Mild fatigue or headache that responds to rest and OTC medications
- Symptoms that improve indoors or after taking an antihistamine
- Known allergy history with familiar, typical symptoms this season
- No significant chest tightness or breathing difficulty
If you’ve been managing symptoms at home for more than 7–10 days without improvement, or if things are getting worse instead of better, that’s your cue to be seen. Chronic untreated allergy inflammation can evolve into sinusitis, ear infections, or worsening asthma.
What Will the ER Actually Do for Allergies?
A lot of people are hesitant to come to the ER for allergy-related symptoms because they think we’ll just tell them to take Benadryl and go home. That’s a misunderstanding of what emergency care looks like when allergies are genuinely impacting your quality of life or safety.
Depending on your presentation, we may:
- Administer IV antihistamines or corticosteroids for severe reactions or allergy-driven asthma flares
- Provide nebulized breathing treatments to open constricted airways
- Give epinephrine (EpiPen-equivalent) if anaphylaxis is suspected
- Run labs to rule out infection, bacterial sinusitis or strep can mimic allergy flares
- Check oxygen saturation and perform chest X-ray if breathing is compromised
- Provide IV fluids if dehydration has set in from prolonged congestion, poor intake, or vomiting
- Help establish a treatment plan and refer to an allergist for longer-term allergy management
What we see frequently at our Fort Worth ER is patients who’ve been suffering through allergy season for weeks with symptoms that never fully resolved, only to discover there was a sinus infection or early asthma complication underneath it all. Don’t assume it’s “just allergies” when it’s persisting.
Seasonal Allergies in Kids: What Parents in Tarrant County Should Know
Children are not small adults when it comes to allergies. Their symptoms can escalate faster, they often can’t tell you clearly how they feel, and their airways are smaller, meaning swelling or inflammation has a more significant effect on their breathing.
Seasonal allergies symptoms in kids often look like a permanent cold during pollen season: constant nose wiping, dark circles under the eyes (allergic shiners), mouth breathing, trouble sleeping, and irritability. If your child has asthma, allergy season is a trigger. Keep their rescue inhaler accessible.
Bring a child to the ER if they’re having difficulty breathing, are working noticeably hard to breathe (ribs visible with each breath, neck muscles straining), or if their lips or fingernails look pale or bluish.
How Long Does Allergy Season Last in Fort Worth?

This is one of the most common questions I hear. And unfortunately, the honest answer for North Texas is: longer than most places. Mountain cedar allergies can peak December through February. Spring brings oak, elm, and ash pollen. Late spring and summer layers in grasses. Fall means ragweed. If you’re sensitized to multiple allergens, which many long-term Fort Worth residents are, you may be symptomatic most of the year.
Individual allergy flares can last anywhere from a few days to several weeks, depending on pollen counts, your medication routine, and how well you’re limiting exposure. If yours is lasting longer than two weeks with no relief, it’s worth being evaluated.
If You’re in Fort Worth and Things Are Getting Worse, We’re Here
Allergy season in North Texas doesn’t care what time it is. If you’ve been trying to manage at home and it’s not working, if your breathing is affected, your child is struggling, or you’re just not sure what’s going on, ER of Fort Worth is open 24 hours a day, 7 days a week, no appointment needed. Come in. We’d rather see you and reassure you than have you wait through something that needed attention sooner.