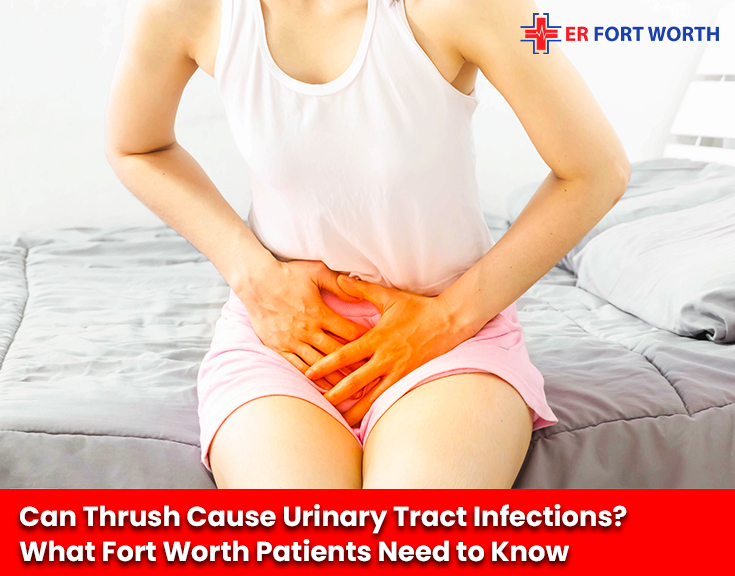
Yes, thrush can cause urinary tract infections, or at least produce symptoms so similar that many patients can’t tell the difference without a lab test. That’s the short answer, and it matters because treating the wrong condition, taking antibiotics for what turns out to be a fungal infection, or waiting on antifungals when you actually have a bacterial UTI, will make things worse, not better.
At our Fort Worth ER, we see this confusion play out regularly. A patient comes in convinced they have a UTI. We run a urinalysis. The bacteria aren’t there, but Candida is. Or the opposite: they’ve been managing what they thought was thrush for two weeks, and the infection has quietly tracked upward toward the kidneys. Both scenarios are avoidable. That’s why we wrote this.
Why Thrush and UTIs Overlap, and How Can Thrush Cause Urinary Tract Infections

Thrush is caused by Candida, a yeast that lives on the skin and mucous membranes of almost every human body. Most of the time it causes no trouble. When it overgrows, though, it causes the itching, discharge, and irritation most people recognise as thrush.
Here’s where it gets complicated. Candida doesn’t always stay put. In some people, particularly those who have recently taken a course of antibiotics, are immunocompromised, or use a urinary catheter, Candida can migrate from the genital area into the urethra and upward into the bladder. When this happens, it’s called candiduria, and the urinary tract infection symptoms it
produces can be nearly identical to a bacterial UTI: burning on urination, pressure in the lower pelvis, frequent urgent trips to the bathroom.
According to the NHS (National Health Service), thrush is caused by an overgrowth of Candida that naturally lives on the skin and mucous membranes. When Candida overgrows in the urinary tract, it can trigger symptoms that closely overlap with a bacterial UTI, which is exactly why laboratory testing is required to confirm the diagnosis.
Research published on PubMed Central confirms that Candida albicans is the leading cause of nosocomial (hospital-acquired) fungal urinary tract infections worldwide, and accounts for a significant proportion of all healthcare-associated UTIs, particularly in patients on broad-spectrum antibiotics or with compromised immune systems.
The takeaway: thrush and UTIs are different conditions, but they share biological territory. And yes, in certain circumstances, one can lead to or mimic the other.
Urinary Tract Infection Symptoms, What They Actually Feel Like
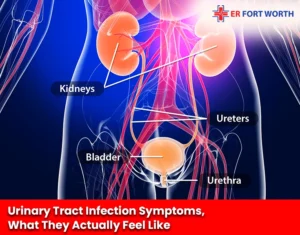
Most articles will give you a bullet list. That’s fine, but it doesn’t prepare you for what a UTI actually feels like at 2 AM when you’re deciding whether to come in.
The burning on urination is sharp, almost stinging, and it often peaks right as the stream finishes. The urgency doesn’t feel like a normal need to go, it’s a cramping, can’t-wait sensation that hits without much warning. You make it to the bathroom and pass very little.
Urinary tract infection pain in the lower back is a specific symptom worth noting separately. If you feel a dull, heavy ache in the area just above your waistline, particularly on one side, that’s your body signalling that the infection may have climbed toward the kidneys. That’s different from simple bladder irritation, and it needs to be evaluated the same day.
Other urinary tract infection symptoms include cloudy or dark urine, a strong ammonia-like odour, and sometimes blood in the urine. Fever, nausea, and chills are less common with a straightforward lower UTI, but when they appear, they indicate an upper urinary tract infection (pyelonephritis) that needs prompt treatment.
Thrush vs UTI, Symptom Comparison Table
This table is designed to help you get a clearer picture before your visit. It’s not a diagnostic tool, a urine culture is the only way to know for certain what you’re dealing with.
| Symptom | Thrush | UTI | Both |
|---|---|---|---|
| Burning on urination | Mild or absent | Yes, often severe | Possible |
| Itching / irritation | Yes, prominent | Mild or absent | Possible |
| Discharge | Thick, white, cottage-cheese-like | Cloudy / strong-smelling urine | Rare |
| Urinary frequency / urgency | Mild, related to irritation | Yes, hallmark symptom | Possible |
| Lower abdominal / pelvic pressure | Uncommon | Yes, common | Possible |
| Lower back / flank pain | Absent | Present (if kidneys involved) | Absent |
| Fever or chills | Absent | Yes, if upper UTI | Absent |
| Nausea | Absent | Yes, if kidneys involved | Absent |
| Odour change | Mild yeasty odour | Strong / ammonia-like urine odour | Possible |
One pattern we see consistently at our Fort Worth ER: patients with thrush tend to report prominent external itching and a cottage-cheese-like discharge, while those with a bacterial UTI lead with the urgency and burning. When you have both at once, which does happen, especially after antibiotic use, lab work is the only way to untangle them.
When Should You Come to the ER Right Now?

Not every UTI or thrush episode needs an emergency room visit. But some do, and waiting can turn a treatable infection into a serious kidney complication. Here’s what we need you to come in for immediately.
- High fever (above 100.4°F / 38°C): This suggests the infection may have reached the kidneys (pyelonephritis). Kidney infections require IV antibiotics and often IV fluids, a course of oral medication at home won’t cut it.
- Urinary tract infection pain in lower back or flank: Sharp or persistent back and side pain alongside UTI symptoms is a kidney-involvement red flag. Don’t wait this out.
- Nausea or vomiting: Nausea accompanying a UTI almost always signals an upper urinary tract infection. If you’re vomiting, you likely can’t keep oral antibiotics down anyway, come in for IV treatment.
- Blood in urine (haematuria): Trace amounts can occur in an uncomplicated UTI, but visible blood, especially in men, warrants same-day evaluation at our Fort Worth ER.
- Confusion or altered mental state: In older adults, a UTI is one of the most common causes of sudden confusion. If an elderly family member suddenly seems disoriented and has urinary symptoms, this is an emergency.
- Symptoms not improving after 48 hours of treatment: If you’re on antibiotics and feel no better after two days, the organism may be resistant, or the diagnosis may be wrong. Come in for a culture.
- Pregnancy: Any UTI symptoms during pregnancy require prompt evaluation without delay. Untreated UTIs in pregnancy carry real risks for both mother and baby.
You can probably wait if: you have mild burning with no fever, you’ve had this before and your regular doctor is available tomorrow, and your symptoms started fewer than 24 hours ago and aren’t getting worse. We’d rather you come in and not need us than stay home and regret it, but we’re also not trying to pull every patient through our doors unnecessarily. That honesty matters to us.
You can access our Fort Worth ER lab testing services around the clock, no appointment needed. A urine culture typically takes minutes to begin and gives us a clear picture of what’s happening and what drug will actually treat it.
Men’s Urinary Tract Infections, What’s Different and Why Men Wait Too Long
We want to address this directly because the internet largely ignores it: men get UTIs. It’s less common than in women, men have a significantly longer urethra, which provides more distance for bacteria to travel before reaching the bladder, but when men develop a UTI, it tends to be more serious.
A men’s urinary tract infection is classified as complicated by default. That’s a clinical term, not a judgment. It simply means that because UTIs are uncommon in men, their presence usually indicates an underlying issue, enlarged prostate, kidney stones, a structural abnormality, or an infection that has already involved the prostate gland (prostatitis) or kidneys.
Symptoms in men can look different from the female presentation. Alongside the usual burning and frequency, men may experience perineal or rectal pain, which signals possible prostate involvement. We see men’s urinary tract infections at our Fort Worth ER more than most people expect, and when they come in, it’s usually after days of assuming it would pass on its own. It rarely does.
If you’re a man in the Tarrant County area experiencing urinary burning, frequency, or pelvic discomfort, especially with fever, come in. Don’t assume it’s something minor. A urine culture and, if indicated, a PSA or prostate exam will give us the full picture quickly.
According to Wikipedia’s entry on urinary tract infections, men’s UTIs are significantly less frequent than those in women but carry a higher risk of complications when they do occur, often involving the upper urinary tract or prostate.
A Clinical Note, Urinary Tract Infection ICD-10 Codes and Diagnosis
For medical professionals and patients reviewing their own records: the primary urinary tract infection ICD-10 code is N39.0 (urinary tract infection, site not specified). Clinicians will also use N30.x for cystitis, N10 for acute pyelonephritis (kidney infection), and, critically for the thrush-UTI overlap, B37.41 for candidal cystitis, which is the specific code for a Candida-caused urinary tract infection.
The distinction between N39.0 and B37.41 matters enormously for treatment. A bacterial UTI coded as N39.0 will be treated with antibiotics. A candidal cystitis coded as B37.41 requires an antifungal, typically fluconazole. Using the wrong treatment class doesn’t just fail, it can worsen the microbiome disruption that caused the problem in the first place.
Diagnosis at our Fort Worth ER starts with a urinalysis and urine microscopy. If Candida is suspected, a urine culture is ordered, this identifies both the organism and, in the case of bacteria, the antibiotic sensitivities. You won’t leave our ER guessing. We give you a clear answer before you go.
What We See in Fort Worth, A Pattern Worth Knowing About
North Texas has its own seasonal patterns that affect this presentation. In Fort Worth, cedar fever season runs hard from November through February. That means a large portion of the Tarrant County population cycles through one or more antibiotic courses every winter, for sinus infections, bronchitis, secondary bacterial complications of the flu.
Antibiotics are brilliant at clearing bacterial infections. They’re equally good at wiping out the beneficial bacteria that keep Candida in check. So what we see at our Fort Worth ER, especially after a run of springtime respiratory infections treated with antibiotics, is a spike in patients presenting with thrush symptoms that have shifted into the urinary tract. It’s not coincidence, it’s microbiology.
Fort Worth families, older adults in Tarrant County, and women on repeated antibiotic courses should know that any urinary symptoms following a recent antibiotic prescription warrant a urine culture, not just a self-diagnosis and an over-the-counter treatment. The culture tells us what’s actually there.
We also see this in Fort Worth patients who have recently been hospitalized. Hospital stays increase catheter use and broad-spectrum antibiotic exposure simultaneously, two of the biggest risk factors for Candida UTIs. If you or a family member develops urinary symptoms within a few weeks of a hospital discharge, that context matters and you should mention it.
Come See Us, We’re Open 24/7 in Fort Worth
If you’re reading this at 11 PM with burning on urination, a fever you can’t explain, or back pain that won’t quit, you don’t have to wait until morning. Our Fort Worth ER is staffed around the clock with physicians who have seen this presentation many times. We run urine cultures on-site, we have IV antibiotics available immediately, and we’ll give you a clear diagnosis before you leave.
No appointment needed. No long wait for basic urinary evaluations. Just experienced ER physicians who want to help you feel better and make sure you’re actually treating the right thing.
Visit us at eroffortworthtx.com or walk in to our Fort Worth location any time, day or night.